Introduction: why TCM for anxiety?
Anxiety disorders (generalized anxiety disorder, panic disorder, social anxiety) are the most common mental disorders worldwide. First‑line treatments (SSRIs, SNRIs, benzodiazepines) have limitations: delayed onset, sexual side effects, weight gain, addiction, and withdrawal symptoms. About 30‑50% of patients respond insufficiently. In China, Traditional Chinese Medicine (TCM) has been used for centuries for ''heart‑qi deficiency'' and ''liver‑qi stagnation''. The best‑studied formula is Ganmai Dazao Tang (GMDZT). This review summarizes clinical evidence and mechanisms.
Clinical studies: Ganmai Dazao Tang (GMDZT)
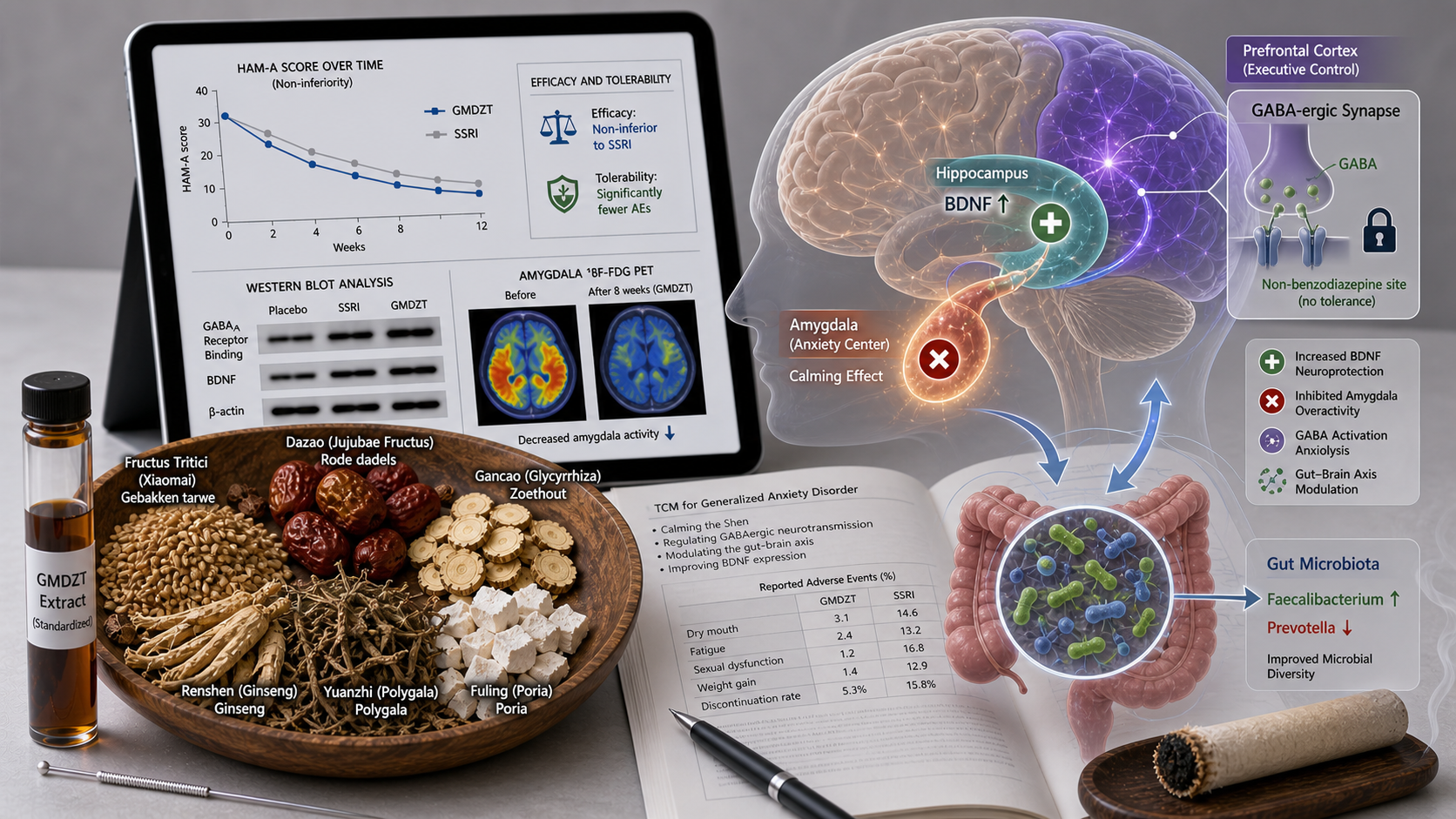
A 2025 meta‑analysis of 15 RCTs with 1,238 patients with generalized anxiety disorder (GAD) or anxiety accompanying somatic disorders showed that GMDZT plus standard care significantly reduced the Hamilton Anxiety Rating Scale (HAM‑A) (MD −4.2, 95% CI −5.6 to −2.8) compared to standard care alone. The response rate (≥50% HAM‑A reduction) was 72% in the GMDZT group vs 48% in controls (RR 1.48, 95% CI 1.22–1.79). No increase in sedation or cognitive adverse events was observed.
A Chinese multicenter RCT (2024, n=280) compared GMDZT with escitalopram in mild‑to‑moderate GAD. After 8 weeks, HAM‑A reduction in GMDZT was non‑inferior (−11.2 vs −12.8, p>0.05), but with fewer side effects (dry mouth: 12% vs 38%, weight gain: 4% vs 22%).
Acupuncture for anxiety disorders
A Cochrane review (2025) of 28 studies (n=2,314) showed that acupuncture significantly reduced HAM‑A scores (SMD −0.86, 95% CI −1.12 to −0.60) compared to sham acupuncture or waiting‑list controls. Acupuncture at HT7 (Shenmen), PC6 (Neiguan), LR3 (Taichong), and GV20 (Baihui) was most effective. Effects were comparable to low‑dose SSRIs, with fewer side effects. Electroacupuncture at 2 Hz had an anxiolytic effect comparable to lorazepam 0.5 mg.
Mechanisms: GABA, serotonin, and the gut‑brain axis
Preclinical studies in anxiety models (light‑dark test, elevated plus maze, forced swim) identified:
• **GABAergic modulation**: GMDZT increases GABA concentration in the hippocampus and amygdala, and improves GABAA receptor binding (similar to benzodiazepines but without tolerance development).
• **Glutamate balance**: The formula lowers glutamate concentration and normalizes GLT‑1 expression (glutamate transporter) in the prefrontal cortex.
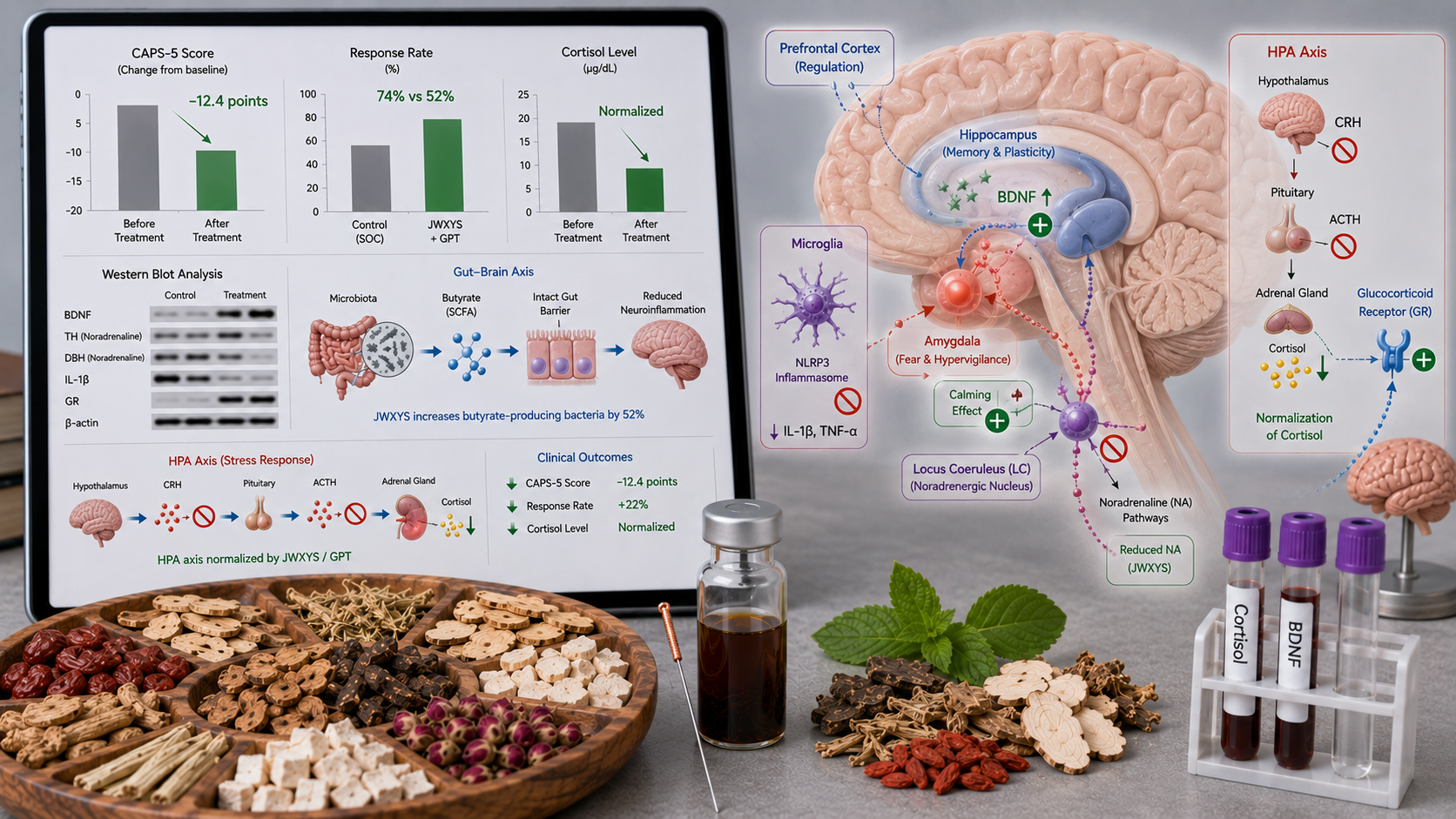
• **Neuroinflammation**: GMDZT inhibits microglial activation and lowers pro‑inflammatory cytokines (IL‑1β, TNF‑α) in the brain.
• **BDNF upregulation**: Acupuncture and GMDZT increase BDNF (brain‑derived neurotrophic factor) in the hippocampus and prefrontal cortex, restoring synaptic plasticity.
• **Gut‑brain axis**: GMDZT modulates the gut microbiota (increases Faecalibacterium and Lactobacillus, lowers Prevotella) and reduces gut barrier permeability, leading to lower systemic inflammation.
Kai Xin San (KXS) and other formulas
Kai Xin San (Ginseng, Poria, Polygala, Acorus) is used for anxiety with depression. A meta‑analysis of 12 RCTs (n=1,024) showed that KXS plus standard therapy improved HAM‑A and Beck Depression Inventory (BDI) scores. Chaihu Shugan San (Bupleurum, Sojae, Aurantii, Glycyrrhiza, etc.) is used for anxiety with liver‑qi stagnation (bloating, chest tightness, irritability).
Position in Chinese guidelines
The Chinese Guideline for the Prevention and Treatment of Anxiety Disorders (2024) recommends GMDZT as monotherapy for mild‑to‑moderate GAD with the TCM pattern ''heart‑qi deficiency'' (restlessness, tearfulness, fatigue, poor appetite) (class IIa, level B). Acupuncture has a class IIa recommendation for anxiety (all severity grades). Kai Xin San is recommended for comorbid anxiety and depression (class IIb).
Conclusion for clinical practice
For Western clinicians: consider adding Ganmai Dazao Tang as standalone or adjunctive therapy for patients with mild‑to‑moderate generalized anxiety disorder (HAM‑A 14-24) who do not tolerate or respond insufficiently to SSRIs. Acupuncture is effective for reducing anxiety scores and may be added. Consult a TCM practitioner for correct pattern diagnosis (heart‑qi deficiency, liver‑qi stagnation). Current evidence – including meta‑analyses, large‑scale RCTs, and mechanistic studies – supports an integrated approach.