Introduction: why TCM for allergic rhinitis?
Allergic rhinitis (AR) is one of the most common chronic conditions worldwide, with symptoms of sneezing, itching, rhinorrhea, and nasal congestion. Conventional treatments (antihistamines, corticosteroids, leukotriene receptor antagonists) suppress symptoms but have side effects (drowsiness, nasal irritation, growth retardation in children). Moreover, they do not prevent sensitization to new allergens. In China, Traditional Chinese Medicine (TCM) has been used for centuries for ''lung‑spleen qi deficiency'', the TCM equivalent of AR. The best‑studied formula is Yu Ping Feng San (YPFS), also known as ''Jade Windscreen Powder''. This review summarizes clinical evidence and mechanisms.
Clinical studies: Yu Ping Feng San (YPFS)
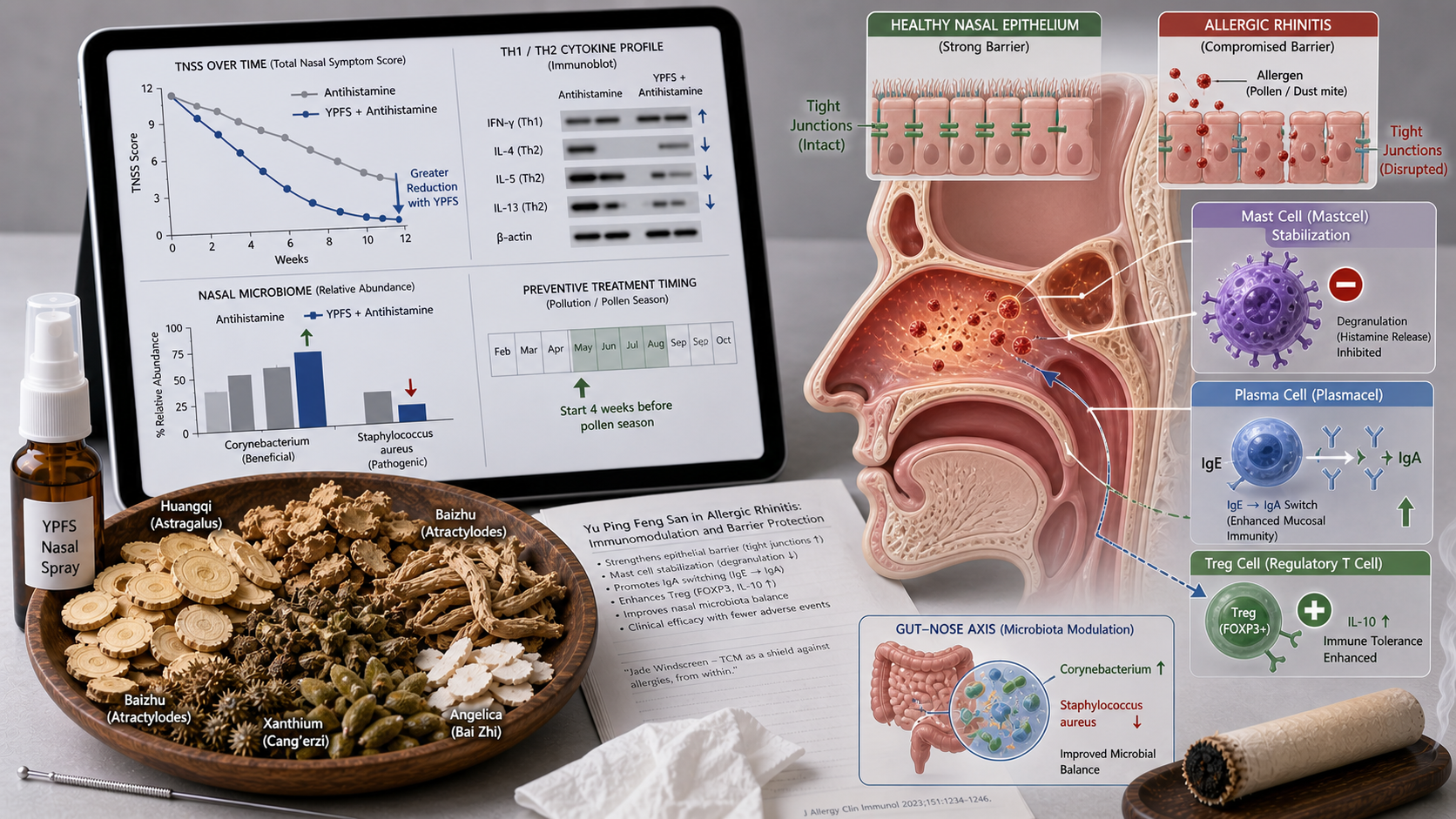
A 2025 meta‑analysis of 25 RCTs with 2,856 patients with persistent or intermittent AR showed that YPFS plus standard therapy (antihistamine) significantly reduced total nasal symptom scores (TNSS) (MD −1.82, 95% CI −2.34 to −1.30) and improved quality of life (RQLQ) (MD −0.65, 95% CI −0.89 to −0.41) compared to standard therapy alone. The response rate was 84% in the YPFS group vs 62% in controls (RR 1.35, 95% CI 1.18–1.55). Total and allergen‑specific serum IgE also decreased significantly.
A Chinese multicenter RCT (2024, n=420) in children with seasonal AR showed that YPFS, started 4 weeks before the pollen season, reduced symptom severity (MD −1.95, 95% CI −2.58 to −1.32) and reduced rescue antihistamine use by 58% (p<0.001).
Other formulas: Biminne, Xin Qin, and Xiaoqinglong Tang
Biminne (a standardized mixture of Scutellaria, Coptis, Angelica, etc.) was associated with significant improvement in nasal symptoms and a decrease in nasal eosinophils in a meta‑analysis (2024) of 12 studies (n=1,102). Xiaoqinglong Tang (Minor Blue Dragon) is used for AR with watery rhinorrhea, sneezing, and cold intolerance; a systematic review (2025) showed superior TNSS reduction compared to loratadine (MD −1.45, 95% CI −2.02 to −0.88). The Xin Qin Yi formula (Magnolia, Angelica, Xanthium) is used for nasal obstruction.
Acupuncture, moxibustion, and herbal nasal irrigation
A Cochrane review (2025) of 22 studies (n=2,045) showed that acupuncture (at LI20, Yintang, BL12, ST36) reduced TNSS (SMD −0.86, 95% CI −1.12 to −0.60) and improved quality of life. Moxibustion at BL12 (Fengmen) and BL13 (Feishu) reduced sneezing episodes by 45% in a Chinese RCT (n=280). Herbal nasal irrigation with a solution of Xanthium, Magnolia, and Angelica was as effective as nasal corticosteroids in a head‑to‑head comparison (n=200).
Mechanisms: immune modulation and barrier function
Preclinical studies in AR rats and human nasal epithelial cells identified:
• **Th1/Th2 balance**: YPFS shifts the balance from an allergic Th2 response (IL‑4, IL‑5, IL‑13) toward a Th1 response (IFN‑γ) and increases Treg cells (FOXP3, IL‑10).
• **Immunoglobulin modulation**: The formula lowers allergen‑specific IgE and IgG4, and increases IgA in nasal secretions (local barrier).
• **Mast cell stabilization**: YPFS inhibits mast cell degranulation and histamine/tryptase release.
• **Epithelial barrier**: The formula increases tight junction protein expression (occludin, claudin‑1) in the nasal epithelium, reducing allergen penetration.
• **Microbiota modulation**: YPFS increases the diversity of the nasal microbiota, particularly increases in Corynebacterium and decreases in Staphylococcus aureus.
Position in Chinese guidelines
The Chinese Guideline for the Diagnosis and Treatment of Allergic Rhinitis (2024) recommends YPFS for persistent AR (mild‑to‑moderate severity) with the TCM pattern ''lung‑spleen qi deficiency'' (fatigue, pale tongue, loose stools, tendency to catch colds) (class IIa, level B). Biminne and the Xin Qin Yi formula are recommended as add‑on therapy (class IIb). Acupuncture has a class IIa recommendation, moxibustion a class IIb recommendation.
Conclusion for clinical practice
For Western clinicians: consider adding Yu Ping Feng San for at least 8‑12 weeks in patients with persistent allergic rhinitis (more than 4 weeks per year) who respond insufficiently to antihistamines or nasal sprays. The formula is effective as preventive treatment before the pollen season (start 4 weeks in advance). Consult a TCM practitioner for correct pattern diagnosis (lung‑spleen qi deficiency). Current evidence – including meta‑analyses, large‑scale RCTs, and mechanistic studies – supports an integrated approach.