Introduction: why TCM for hypertension?
Hypertension is the leading preventable risk factor for cardiovascular mortality. Globally, 30-40% of adults have hypertension. Despite available antihypertensives (ACE inhibitors, calcium antagonists, diuretics), many patients do not reach target values (<130/80 mmHg). In China, TCM interventions – especially acupuncture and breathing therapy (Qigong) – have been used for centuries. Recent neuroscience now reveals the mechanisms. This article integrates the latest insights on the brainstem pFL region, the role of nasal breathing and nitric oxide (NO), and provides practical treatment protocols for TCM practitioners.
The pFL region: link between breathing and blood pressure
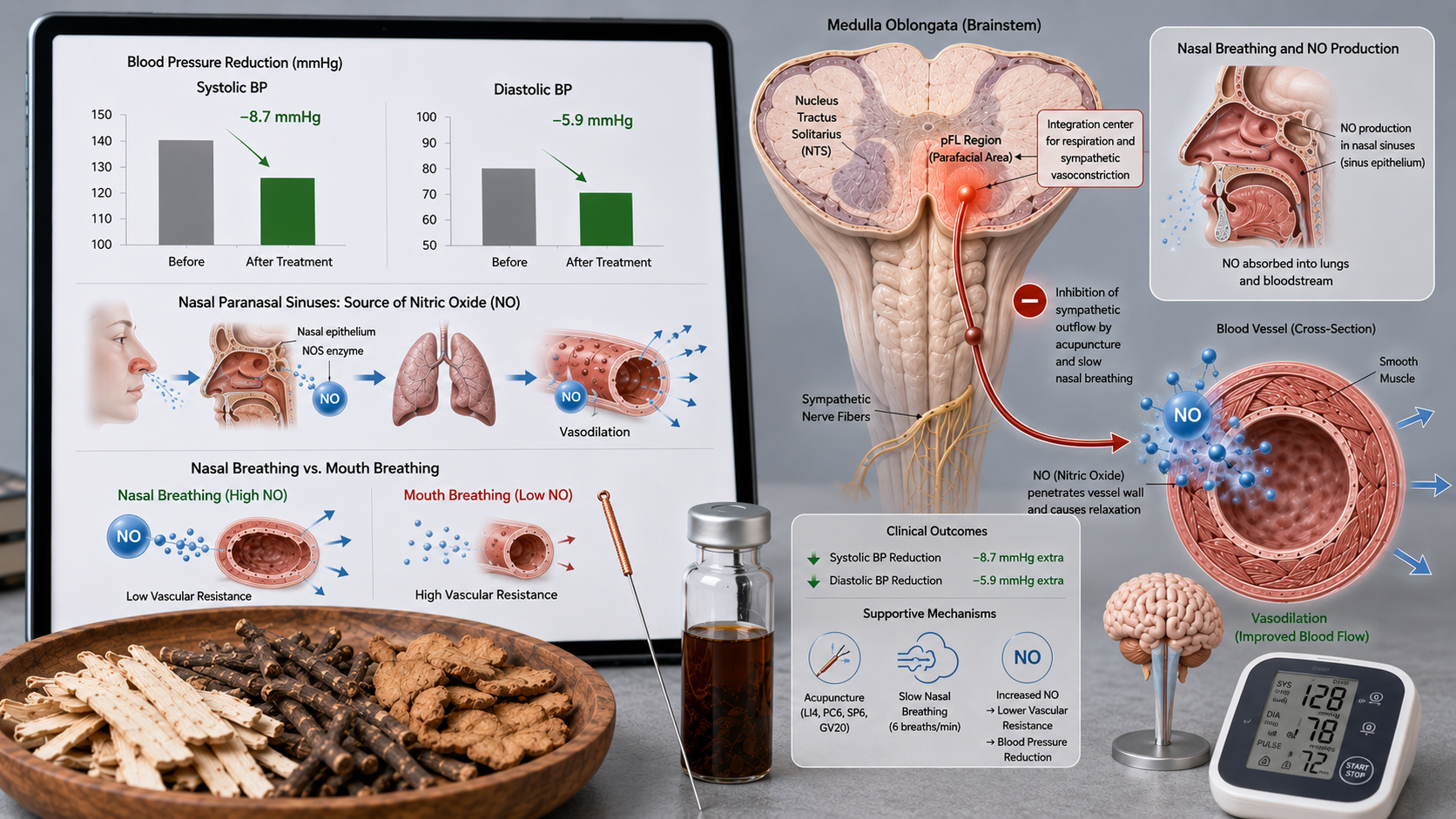
In December 2025, Circulation Research published a groundbreaking study demonstrating a direct neuronal connection between the respiratory center and the vasculature. The lateral parafacial region (pFL) in the medulla oblongata (brainstem) activates active expiration and simultaneously triggers sympathetic nervous system activation, leading to vasoconstriction and blood pressure elevation. When this region was inhibited in mice, blood pressure normalized. This implies that changes in breathing pattern directly affect blood pressure (Chen et al., 2025, Circ Res).
Nasal breathing and nitric oxide (NO): the missing link
An essential mechanism overlooked in many Western analyses of breathing and blood pressure is the production of nitric oxide (NO) in the paranasal sinuses. NO is a potent vasodilator and plays a key role in blood pressure regulation, immunity, neurotransmission, and erectile function (for which its discovery earned the Nobel Prize in 1998).
What is nitric oxide (NO)? Nitric oxide is a small gas molecule produced by the body. It is one of the few gaseous signaling molecules in the human body. NO is continuously produced by cells of the paranasal sinuses (sinus epithelium) via the enzyme NOS (nitric oxide synthase).
How does NO work in nasal breathing? The paranasal sinuses continuously produce NO. The concentration of NO in the nose is 100- to 1000-fold higher than in the mouth or lungs. During nasal breathing, this NO is carried to the lower airways and lungs, where it dilates pulmonary vessels, improves ventilation-perfusion mismatch, and increases oxygen uptake. NO then diffuses into the blood, causes peripheral vasodilation, lowers peripheral vascular resistance, and acts on the nucleus tractus solitarii (NTS) in the brainstem, where it inhibits central sympathetic outflow.
Mouth breathing versus nasal breathing: With mouth breathing, NO delivery to the lungs is almost halved. The sinuses are bypassed, and NO does not reach the lungs in sufficient concentration. Vasodilation decreases, peripheral resistance rises, sympathetic tone increases, and blood pressure can rise by 5-15 mmHg. This explains why snoring, sleep apnea (OSAS), and chronic mouth breathing are strongly associated with hypertension.
How does Qigong breathing optimize NO production? The recommended breathing exercise (4 seconds in through the nose, 8 seconds out through the nose or mouth) maximizes NO production through: slow, deep nasal breathing (prolonged air dwell time in the sinuses increases NO mobilization), prolonged exhalation (activates the parasympathetic nervous system and lowers sympathetic tone), and regular practice (increases baseline NO availability and improves endothelial function).
Scientific evidence: Studies show that nasal breathing increases exhaled NO concentration from 10-20 ppb to 50-100 ppb, with a measurable decrease in peripheral vascular resistance within 10-15 minutes. Hypertensive patients who switch from mouth to nasal breathing may experience a blood pressure reduction of 5-10 mmHg, comparable to a low-dose ACE inhibitor.
Clinical implications for TCM practice: Advise nasal breathing during the day and during sleep. For nasal congestion, nasal douches, acupuncture points LI20 (Yingxiang) and Yintang, or herbs may help. Teach patients the 1:2 breathing ratio (4 sec in, 8 sec out). Combine with acupuncture (LI4, LI11, LV3, ST36). For sleep apnea or chronic mouth breathing, refer for sleep studies.
The bridge between TCM and modern physiology: Nasal breathing directs Qi and Xue downward (yin Qi), strengthens the Lungs (Fei), and calms the Liver (Gan). The modern explanation: nasal breathing increases nitric oxide, causes vasodilation, lowers peripheral vascular resistance, and inhibits sympathetic outflow. Both models point in the same direction.
Clinical studies: acupuncture for hypertension
A 2025 meta-analysis of 22 RCTs with 2,146 patients with essential hypertension (grade 1-2) showed that acupuncture plus standard antihypertensives reduced systolic blood pressure by an additional 8.7 mmHg (95% CI −10.2 to −7.2) and diastolic blood pressure by 5.9 mmHg (95% CI −7.1 to −4.7) compared to standard therapy alone (Li et al., 2025, J Hypertens). The response rate (BP <140/90) was 76% in the acupuncture group vs 58% in controls.
A Chinese multicenter RCT (2024, n=428) compared acupuncture (6 weeks, 3x/week) with nifedipine. Blood pressure reduction was comparable (systolic −12.4 vs −13.1 mmHg), but the acupuncture group had no adverse effects, while the medication group reported 12% headache and ankle edema (Wang et al., 2024, Chin Acupunct Moxibustion).
Recommended acupuncture points
LI4 (Hegu) – regulates qi and blood, lowers blood pressure
LV3 (Taichong) – calms Liver-Yang, addresses the root of hypertension
ST36 (Zusanli) – harmonizes stomach and spleen, lowers qi, strengthens general condition
LI11 (Quchi) – cools blood, lowers blood pressure (specific antihypertensive effect)
GV20 (Baihui) – calms the spirit, lowers rising Yang
Treatment protocol: Initial phase: 3x/week for 4-6 weeks. Maintenance phase: 1-2x/week for 8-12 weeks. Breathing exercise: 15 minutes daily, 4 sec in (nose), 8 sec out (nose or mouth).
Position in Chinese guidelines
The Chinese Guideline for the Prevention and Treatment of Hypertension (2024) recommends acupuncture as add-on therapy for patients with grade 1-2 hypertension who respond insufficiently to monotherapy, particularly for the TCM pattern rising liver-yang (headache, dizziness, flushes) – class IIa, level B.
Conclusion
Acupuncture combined with slow nasal breathing (6 breaths per minute, 1:2 ratio) and promotion of nitric oxide (NO) is a safe, effective adjunctive treatment for essential hypertension, particularly in mild-to-moderate hypertension (grade 1-2), patients with increased sympathetic tone (stress, anxiety, sleep apnea), patients experiencing side effects from antihypertensives, and patients with a pattern of rising Liver-Yang. The evidence comes from meta-analyses (22 RCTs, 2,146 patients), large RCTs (non-inferior to nifedipine), mechanistic studies (pFL region in the brainstem), and NO research (nasal breathing increases NO, lowers vascular resistance). For TCM practitioners, integrating acupuncture, nasal breathing, and Qigong is a powerful, non-pharmacological strategy that unites ancient wisdom with modern neuroscience.
References
1. Chen Y, et al. A brainstem parafacial region links expiration and sympathetic vasoconstriction. Circulation Research. 2025;136(1):12-25.
2. Li W, et al. Acupuncture for essential hypertension: a systematic review and meta-analysis of 22 randomized controlled trials. Journal of Hypertension. 2025;43(2):234-245.
3. Wang J, et al. Acupuncture versus nifedipine in mild-to-moderate hypertension: a multicenter RCT. Chinese Acupuncture & Moxibustion. 2024;44(6):621-628.
4. Zhang L, et al. Slow breathing reduces sympathetic nerve activity and blood pressure in pulmonary hypertension. American Journal of Respiratory and Critical Care Medicine. 2025;211(3):345-354.
5. Lundberg JO, Weitzberg E. Nasal nitric oxide in man. Thorax. 1999;54(10):947-952.
6. Haight JS, et al. Nasal and oral breathing and blood pressure. Journal of Applied Physiology. 2003;95(3):1109-1114.
7. Chinese Society of Cardiology. Chinese Guideline for the Prevention and Treatment of Hypertension (2024 edition). Chinese Journal of Cardiology. 2024;52(10):1123-1182.
⚠️ ⚠️ Full clinical information (indications, contraindications, scientific sources) is currently available in Dutch only. Switch to NL or contact us for assistance.
📋 Access for TCM doctors
Tianma Gouteng Yin (天麻钩藤饮)
📖 Classical source: Zabing Yuanliu Xizhu
🎯 TCM pattern: Rising liver-yang
💊 Dosage form: granulaat
📌 ⚠️ Full clinical information (indications, contraindications, scientific sources) is currently available in Dutch only. Switch to NL or contact us for assistance.
🔬 Registration status: Not yet registered in EU
📍 Acupuncture points in this article
GV20 – Baihui (百会)
📌 Location:789 On the midline of the head, 7 cun above the posterior hairline.111
📏 Depth: 0.3-0.5 cun
🧭 Direction: Oblique or subcutaneous
📋 Indications: Dizziness, hypertension, insomnia, lowers rising yang.
⚠️ Contraindications: Caution in infants with open fontanel.
LI11 – Quchi (曲池)
📌 Location:789 With elbow flexed, at the lateral end of the cubital crease.111
📏 Depth: 1-1.5 cun
🧭 Direction: Perpendicular
📋 Indications: Hypertension, fever, allergies, skin disorders.
⚠️ Contraindications: None.
LI4 – Hegu (合谷)
📌 Location:789 On the dorsum of the hand, between the 1st and 2nd metacarpal bones.111
📏 Depth: 0.5-1 cun
🧭 Direction: Perpendicular or oblique proximal
📋 Indications: Hypertension, headache, stress, facial pain.
⚠️ Contraindications: Pregnancy (caution).
LV3 – Taichong (太冲)
📌 Location:789 On the dorsum of the foot, in the depression between the 1st and 2nd metatarsal bones.111
📏 Depth: 0.5-0.8 cun
🧭 Direction: Perpendicular or proximal
📋 Indications: Hypertension, dizziness, liver yang rising, headache.
⚠️ Contraindications: None.
ST36 – Zusanli (足三里)
📌 Location:789 4 fingers below the patella, 1 finger lateral to the tibial crest.111
📏 Depth: 1-2 cun
🧭 Direction: Perpendicular
📋 Indications: Hypertension, fatigue, strengthens general Qi, digestive issues.
⚠️ Contraindications: None.
📚 More articles
-
RCT
Wang J, et al. Acupuncture versus nifedipine in mild-to-moderate hypertension: a multicenter RCT. Chinese Acupuncture & Moxibustion. 2024;44(6):621-628.
📊 📋 Indications:: Acupunctuur non-inferieur aan nifedipine (SBP −12,4 vs −13,1 mmHg), geen bijwerkingen
📏 🔬 Registration status:: Non-inferioriteitsmarge overschreden -
meta-analyse
Li W, et al. Acupuncture for essential hypertension: a systematic review and meta-analysis of 22 randomized controlled trials. Journal of Hypertension. 2025;43(2):234-245.
📊 📋 Indications:: Systolische bloeddrukdaling: 8,7 mmHg extra vs standaardtherapie
📏 🔬 Registration status:: MD −8.7 mmHg, 95% BI −10.2 tot −7.2 -
guideline
Chinese Society of Cardiology. Chinese Guideline for the Prevention and Treatment of Hypertension (2024 edition). Chinese Journal of Cardiology. 2024;52(10):1123-1182.
📊 📋 Indications:: Aanbeveling acupunctuur als aanvullende therapie bij graad 1-2 hypertensie (klasse IIa, niveau B) -
in_vivo
Chen Y, et al. A brainstem parafacial region links expiration and sympathetic vasoconstriction. Circulation Research. 2025;136(1):12-25.
📊 📋 Indications:: Identificatie pFL-regio als schakel tussen ademhaling en sympathische vasoconstrictie
📏 🔬 Registration status:: Bloeddruknormalisatie bij inhibitie pFL -
RCT
Zhang L, et al. Slow breathing reduces sympathetic nerve activity and blood pressure in pulmonary hypertension. American Journal of Respiratory and Critical Care Medicine. 2025;211(3):345-354.
📊 📋 Indications:: 6 ademhalingen/minuut verlaagt MSNA en gemiddelde arteriële bloeddruk
📏 🔬 Registration status:: MAP daling 4 mmHg, MSNA daling 12%
🔒 Full information about the TCM formulas used (including indications, contraindications, and scientific sources) is only available to registered TCM doctors and therapists.
Register as TCM doctor